The information in this brief is intended for educational use only.
This brief provides a summary of the CHOICES Learning Collaborative Partnership simulation model of integrating the Nutrition and Physical Activity Self-Assessment for Child Care (NAP SACC) into Washington’s Quality Rating and Improvement System (QRIS), Early Achievers, which awards quality ratings to early care and education (ECE) programs meeting defined standards.
The Issue
Over the past three decades, more and more people have developed obesity.1 Today, nearly nine percent of 2-5 year olds have obesity.2 Health care costs for treating obesity-related health conditions such as heart disease and diabetes were $147 billion in 2008.3 Emerging prevention strategies directed at children show great promise for addressing this issue.4 A large body of evidence shows that healthy eating, physical activity, and limited screen media time (like watching TV or smartphones) helps kids grow up at a healthy weight.
In Washington, over a quarter of 2-5 year olds attend a licensed ECE program.5 Because QRIS systems like Early Achievers incentivize ECE programs to meet high standards and provide training, they are an ideal way to help ECE programs engage in improving nutrition, physical activity, and screen time practices. The Department of Early Learning invested $91 million in Early Achievers in 2016-17.5
About NAP SACC and QRIS
NAP SACC, based on the best available scientific evidence, helps ECE providers improve nutrition, active play, and screen time practices.6,7 QRIS programs encourage providers to improve in quality by using a voluntary and rewarding (rather than regulatory and punitive) approach and offers a mechanism for implementing a time-intensive program like NAP SACC. ECE directors complete self-assessments of existing practices and receive training and technical assistance to implement changes that create healthier environments. In Washington’s hypothetical model, completing NAP SACC would be an option for ECE providers seeking to achieve Early Achievers Level 3 status. State-contracted coaches would train providers and conduct technical assistance for meeting NAP SACC goals.
Comparing Costs and Outcomes
CHOICES cost-effectiveness analysis compared the costs and outcomes of integrating NAP SACC into Early Achievers over 10 years (2015-2025) with costs and outcomes associated with not implementing the program. The approach assumes that 72% licensed ECE centers participate in Early Achievers, and 25% of both center-based and home-based providers adopt NAP SACC.
| Implementing NAP SACC in child care programs throughout Washington is an investment in the future. By the end of 2025: 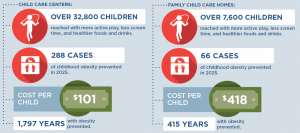 |
Conclusions and Implications
Every child deserves a healthy start in life. This includes ensuring that all kids in child care have opportunities to eat healthy foods and be physically active, no matter where they live or where they go for child care. A state-level initiative to bring the NAP SACC self-assessment and improvement process to Washington child care programs through the Early Achievers system could prevent over a thousand cases of childhood obesity in 2025 and ensure healthy child care environments for over 160,000 children. For every $1 spent implementing this strategy with child care centers, we would save $0.08 in health care costs as a result of decreased obesity prevalence. For every $1 spent implementing this strategy with family home providers, we would save $0.02 in health care costs as a result of decreased obesity prevalence
These results reinforce the importance of investing in prevention efforts, to reduce the prevalence of obesity. Shortchanging prevention efforts can lead to more costly and complicated treatment options in the future. Introducing small changes to young children can help them develop healthy habits for life.
Evidence is growing about how to help children achieve a healthy weight. Programs such as NAP SACC are laying the foundation for healthier generations by helping ECE providers create environments that nurture healthy habits. Leaders at the federal, state, and local level should use the best available evidence to help children eat healthier diets and be more active.
References
- Flegal, K.M., Kruszon-Moran, D., Carroll, M.D., Fryar, C.D., Ogden, C.L. (2016). Trends in Obesity Among Adults in the United States, 2005 to 2014. JAMA, 315(21), 2284-91.
- Ogden, C. L., Carroll, M. D., Lawman, H. G., Fryar, C. D., Kruszon-Moran, D., Kit, B. K., & Flegal, K. M. (2016). Trends in obesity prevalence among children and adolescents in the United States, 1988-1994 through 2013–2014. JAMA, 315(21), 2292-2299.
- Finkelstein EA, Trogdon JG, Cohen JW, Dietz W. Annual Medical Spending Attributable To Obesity: Payer-And Service-Specific Estimates. Health Affairs. 2009;28(5).
- Gortmaker, S. L., Wang, Y. C., Long, M. W., Giles, C. M., Ward, Z. J., Barrett, J. L., …Cradock, A. L. (2015). Three interventions that reduce childhood obesity are projected to save more than they cost to implement. Health Affairs, 34(11), 1932–1939.
- DEL Early Achievers Data Dashboard and Market Rate Report, June 2015; Early Start Act Report.
- Ward, D.S., Benjamin S.E., Ammerman, A.S., Ball, S.C., Neelon, B.H., Bangdiwala, S.I. (2008). Nutrition and physical activity in child care: results from an environmental intervention. Am J Prev Med, 35(4):352-6.
- Alkon, A., Crowley, A.A., Neelon, S.E., Hill, S., Pan, Y., Nguyen, V., Rose, R., Savage, E., Forestieri, N., Shipman, L., Kotch, J.B. (2014). Nutrition and physical activity randomized control trial in child care centers improves knowledge, policies, and children’s body mass index. BMC Public Health, 14:215.
Suggested Citation:Cradock AL, Gortmaker SL, Pipito A, Kenney EL, Giles CM. Washington: NAP SACC: Researching an Intervention to Create the Healthiest Next Generation [Issue Brief]. Washington State Department of Health, Olympia, WA, and the CHOICES Learning Collaborative Partnership at the Harvard T.H. Chan School of Public Health, Boston, MA; August 2017. |
The design for this brief and its graphics were developed by Molly Garrone, MA and partners at Burness.
This issue brief was developed at the Harvard T.H. Chan School of Public Health in collaboration with the Washington State Department of Health through participation in the Childhood Obesity Intervention Cost-Effectiveness Study (CHOICES) Learning Collaborative Partnership. This brief is intended for educational use only. Funded by The JPB Foundation. Results are those of the authors and not the funders. For more information, please visit: http://www.doh.wa.gov/CommunityandEnvironment/HealthiestNextGeneration/CHOICES
